 
You typically can't eat or drink anything for about eight hours before cardioversion. During that time, you'll usually take blood thinners to reduce the risk of complications. If you have one or more blood clots in the heart, cardioversion is typically delayed for 3 to 4 weeks. Your provider will decide whether you need this test before cardioversion. Cardioversion can make blood clots move, causing life-threatening complications. If irregular heart rhythm symptoms are severe, cardioversion may be done in an emergency setting.īefore cardioversion, you may have an imaging test called a transesophageal echocardiogram to check for blood clots in the heart. How you prepareĬardioversion is usually scheduled in advance. Rarely, some people get minor burns on their skin from the sensors (electrodes).Ĭardioversion can be done during pregnancy, but it's recommended that the baby's heartbeat be monitored during the procedure. Medications or additional shocks can be given to correct the heart's rhythm. If it happens, it usually occurs minutes after the procedure. Rarely, some people develop other irregular heartbeats during or after cardioversion. Some people may be given blood thinners before the procedure. This can cause life-threatening complications, such as a stroke or a blood clot traveling to your lungs.Ī health care provider may order tests to check for blood clots before doing cardioversion. Shocking the heart can cause these blood clots to move to other parts of the body. Some people who have irregular heartbeats, such as A-fib, have blood clots form in the heart. Potential risks of electric cardioversion include:ĭislodged blood clots. Your health care provider can take steps to reduce your risk. It has been updated.ĭownload a copy of the guide: 10 tips to identify atrial flutter.Complications of cardioversion are uncommon. 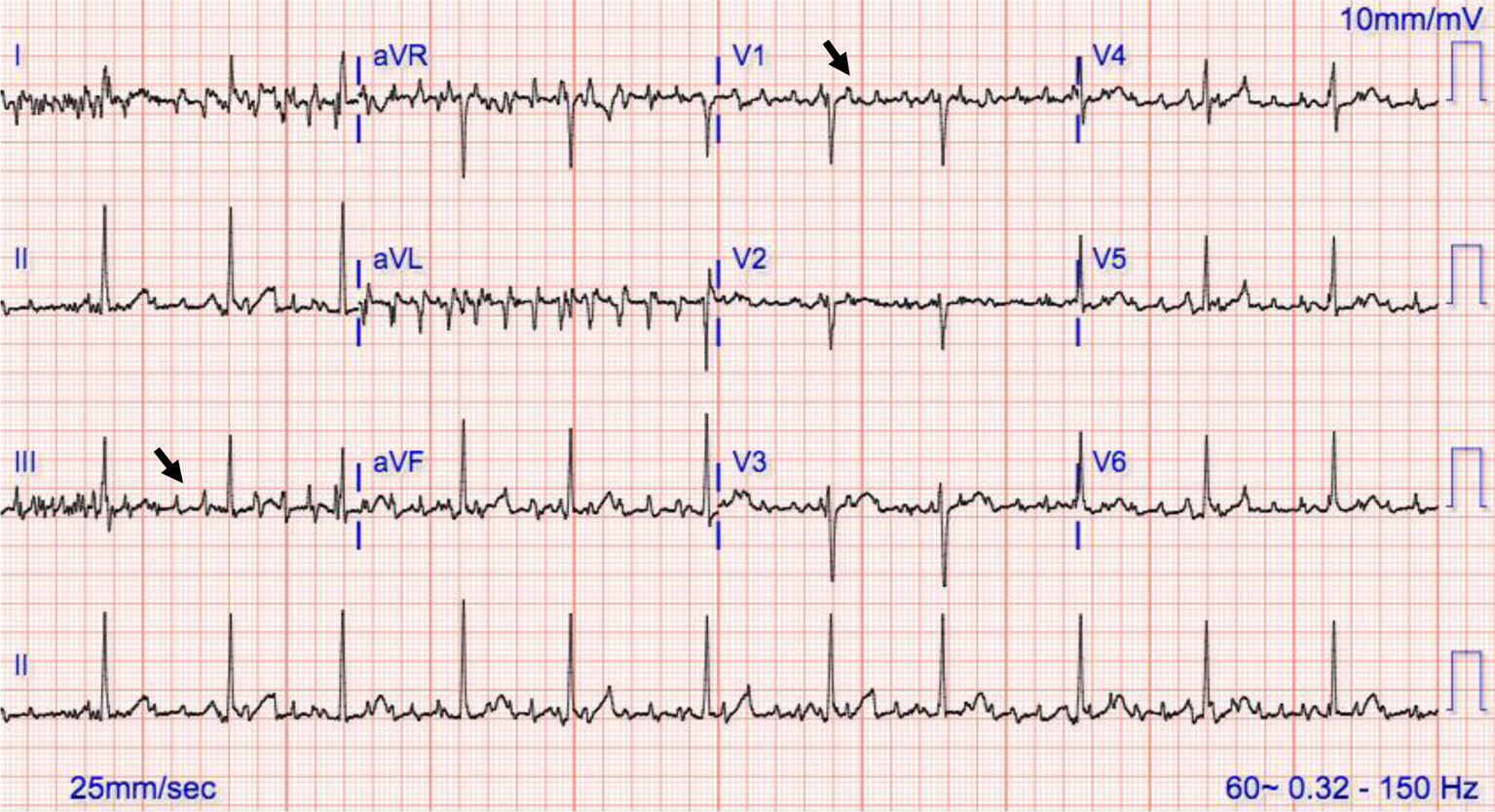
Read next: Training Day: Mastering the 12-lead With these tips and practice, you will be much less likely to mistake atrial flutter with 2:1 conduction for another tachycardia. You will learn to see the rhythm strip as separate atrial activity and ventricular activity portions and the hidden flutter waves will stand out for you. Look at as many strips of confirmed 2:1 conduction as you can and your eye will become trained to see it. Now that you are more aware of atrial flutter with 2:1 conduction, the best way to get good at recognizing it is regular practice. You might consider using a Lewis lead, which enhances detection of atrial activity. In some leads, atrial flutter will not have a sawtooth pattern. A 12-lead ECG can help immensely in seeing the flutter waves, because some leads are better for viewing atrial activity than others. Use more than one leadįor rhythm interpretation, the more leads the better. By evaluating the P waves, QRS complexes, intervals and rate, you may discover that your first impression was wrong. Get your first impression, then think of alternate diagnoses and apply rhythm interpretation criteria. Most people with sinus tach, especially over 130 bpm, will usually have a readily-apparent reason for the tachycardia, like fever, fear, pain, anxiety, exertion, drugs, hypovolemia or hypoxia. You see no obvious reason for sinus tachycardiaĬonsider atrial flutter if the patient has no obvious reason for sinus tachycardia. 
Re-entrant tachycardias hit a fast rate suddenly and maintain that rate until they end suddenly. For example, if your patient talks or moves around in bed, the rate may go up slightly. Remember that sinus rhythms tend to fluctuate slightly. 
Suspect any tachycardiaĪny rhythm around 150 bpm should be suspected of being atrial flutter with 2:1 conduction. Here are 10 tips to avoid missing atrial flutter. You won't find atrial flutter it if you aren’t looking for it. 10 tips to avoid missing atrial flutter with 2:1 conduction. As cardiac output is decreased and cardiac workload increased, ventricular fibrillation can result. In patients with accessory pathways that bypass the slow conduction of the AV node, like Wolff-Parkinson-White Syndrome, 1:1 conduction of atrial flutter or atrial fib can be life-threatening. Atrial flutter can lead to fast rates at 2:1 conduction, and VERY fast rates at 1:1 conduction. When we see slower ventricular rates and conduction ratios of 3:1 or more, it is usually due to medications or other causes of enhanced refractoriness of the AV node. New-onset atrial flutter is most often conducted 2:1, because that is a comfortable rate (around 150 per minute) for the AV node to conduct. The AV node is bombarded by a regular atrial rhythm of around 300 per minute. It can occur suddenly, and is sometimes associated with periods of atrial fibrillation. Atrial flutter is a re-entrant tachycardia that occurs in the atria. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
